The Stages of ACL Graft Healing
Recovering from an anterior cruciate ligament (ACL) reconstruction is a major physical and mental journey. As a patient, you likely want to know exactly when you can return to the sports and daily activities you love. It is completely natural to feel eager to get moving again. However, pushing your body too hard and too soon can severely jeopardise your new ligament and set your recovery back by months.
Understanding the ACL graft healing timeline is critical for a safe, successful, and long-lasting recovery. Your new graft does not just magically attach to your bone and work flawlessly right away. Instead, it undergoes a highly complex biological transformation inside your knee. Knowing exactly what happens beneath the surface helps you make smart, informed choices about your rehabilitation.
In this comprehensive guide, we will explore the crucial key takeaways of your healing journey. We will break down the key stages of ACL recovery, highlight the timeline of your biological healing process, and explain exactly when your graft is most vulnerable to damage. By the time you finish reading, you will have a clear, actionable roadmap for protecting your knee and achieving a full recovery.
Key Stages of Healing: Understanding Your ACL Recovery
When you undergo ACL reconstruction, the graft acts as a scaffold that undergoes a complex biological transition known as “ligamentisation.” During this remarkable process, the piece of tendon tissue used to replace your torn ACL transforms into a living, functioning ligament.
Because a tendon is structurally different from a ligament, your body must break it down and rebuild it to suit its new purpose. We can break this ACL graft healing timeline into four distinct phases, each requiring a specific approach to care and rehabilitation.
Weeks 0 to 4: Initial Healing and Protection
Immediately following your orthopaedic surgery, your knee will experience significant swelling, stiffness, and inflammation. Do not be alarmed; this is a completely normal part of your body’s acute healing response. During this initial stage, the newly placed graft is essentially dead tissue but is structurally stronger than your ruptured ACL. It has no blood supply of its own, and it is held in place entirely by the surgical fixation devices, such as screws, buttons, or staples, used during your operation.
Your primary goals during these first four weeks are straightforward but essential. You must focus on managing your pain, reducing joint swelling, preventing muscle loss and gently restoring your range of motion.
You will likely use crutches to assist with walking and may wear a brace to protect the joint from unexpected movements. Your physiotherapist will guide you through gentle isometric exercises to “wake up” your quadriceps without stressing the new graft.
Weeks 4 to 12: The Proliferation/Revascularisation Phase
As you move into the second month of your recovery, the acute inflammation and deep aching usually settle down. Biologically, the original cells within the graft tissue begin to die off completely, and your body starts to build brand new blood vessels into the graft to supply it with nutrients.
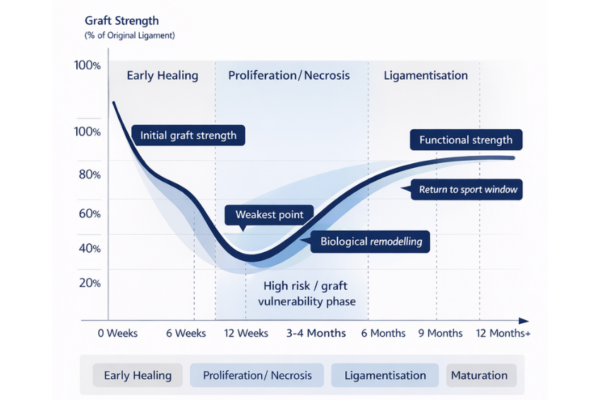
This phase is notoriously deceptive. From the outside, your knee might look and feel much better. Your day-to-day pain may entirely vanish, and you might find walking quite easy. However, inside the joint, the graft is undergoing a massive structural overhaul. Your body is laying down the blood vessels necessary to remodel the graft. This starts from the bone sockets, called tunnels, and proceeds inwards toward the middle of the tendon graft. The incorporation into the bone sockets is quicker with bone-patella tendon-bone grafts and is slowest with allograft or donor graft tissue. The graft is generally at its weakest at about 6-12 weeks post-surgery and vulnerable to stretching, micro tears or even complete rupture. Caution must be taken during this period.
This intense biological activity renders the graft’s structural integrity highly vulnerable to physical stress, which we will explore in detail shortly.
Months 3 to 6 (up to 9 months): Graft Integration and Ligamentisation
By the third month, the new blood supply is firmly established. Your body begins laying down fresh collagen fibres over the graft scaffold, and the graft slowly starts to look, feel, and behave more like a natural human ligament.
During this stage of the ACL graft healing timeline, your rehabilitation takes a noticeable step forward. You will focus heavily on rebuilding functional muscle strength, particularly targeting your quadriceps, hamstrings, and calves.
Under the strict guidance of your physiotherapist, you can usually begin light, straight-line jogging. You will also introduce more advanced strengthening exercises, balance work, and proprioception drills. While the graft is getting stronger, it is still not ready for unpredictable, high-impact sports.
Month 9 and Beyond: Full Recovery
In the final stages of the healing process, the graft continues to mature, thicken, and strengthen. The new collagen fibres organise themselves systematically to handle the specific mechanical loads placed on the knee during dynamic movement.
During these months, you will slowly transition into sport-specific drills. This includes agility training, hopping, jumping, and eventual pivoting movements. Achieving full recovery and receiving clearance to return to competitive sports typically happens between 9 and 12 months post-surgery. However, this timeline depends entirely on you meeting specific physical milestones, rather than simply crossing dates off a calendar. Your surgical and rehabilitation team will test your strength, stability, and confidence before giving you the final green light.
When is the ACL Graft Weakest? The Danger Zone
A common and incredibly crucial question that patients ask their specialists is: When is the ACL graft weakest?
It is reasonable to assume that your knee is weakest the day after your surgery. However, biological studies indicate that the graft is most vulnerable between 6 and 12 weeks post-surgery. Orthopaedic professionals frequently refer to this specific window as the “danger zone.”
To understand why this happens, we must look at the biology of ligamentisation. When the surgeon inserts the graft, it is essentially a strong, dense piece of tendon, stronger than the native ligament you ruptured. As the weeks progress, the graft undergoes a process called necrosis.
During necrosis, the tissue loses its original mechanical strength because the body actively breaks it down to build a new blood supply and cellular structure. The new ligament has not yet developed its own internal structural integrity.
This creates a highly dangerous mismatch for the patient. By weeks 6 to 8, many people have regained full motion, and the knee feels fantastic. The initial surgical swelling is gone, walking feels normal, and confidence is soaring. Because they feel so good, patients are often tempted to test their limits.
Doing so during this peak vulnerability period places immense, unmanageable stress on a structurally fragile graft. Even a minor misstep can stretch the healing tissue or, in the worst-case scenario, cause a complete re-rupture. Understanding this invisible weakness is your absolute best defence against a devastating setback. You must respect the biology, even when your body tells you that you are ready for more.
Practical Tips for Recovery: Protecting Your New ACL
Navigating the ACL graft healing timeline requires an abundance of patience, discipline, and mental fortitude. It is a marathon, not a sprint. Here is practical, actionable advice to help you protect your knee, especially when the graft is at its weakest.
Stick Strictly to Your Physiotherapy Programme
Your physiotherapist designs your exercise routine based on the specific biological healing stages of your graft. Never skip ahead to more advanced exercises just because your knee feels good on a particular day. Stick strictly to the prescribed movements, sets, and repetitions. Consistency in your approved exercises builds the surrounding muscle strength needed to absorb shock and protect the joint, acting as an internal shock absorber for your fragile new ligament.
Modify Your Daily Activities
You must avoid any sudden twisting, pivoting, or jumping until your orthopaedic surgeon and physiotherapist explicitly clear you for these movements. If you are walking on uneven surfaces, wet grass, or in crowded areas during the first few months, remain highly vigilant. A simple slip, a sudden change of direction to avoid someone walking toward you, or an unexpected stumble can place dangerous rotational tension on the healing tissue.
Prioritise Sleep and Nutrition
Healing a major ligament and rebuilding muscle tissue requires a tremendous amount of internal energy. You must provide your body with the right fuel. Eat a balanced diet rich in lean protein, healthy fats, vitamins, and minerals to support cellular tissue repair.
Equally importantly, ensure you get enough high-quality sleep. Your body does the vast majority of its cellular repair while you are resting in deep sleep. Skimping on sleep can directly slow down your biological healing timelines.
Listen to Your Body and Avoid Comparisons
Every single body heals at a slightly different rate. Do not compare your recovery timeline to a professional athlete you saw on television, or even a friend who had the same surgery. If your knee swells after a specific exercise, or if you feel a deep ache, listen to those signals. Back off the intensity, apply ice, and communicate these changes to your physiotherapist.
Your Path to Recovery
Successfully navigating your ACL recovery stages requires a delicate balance of targeted hard work and strategic, unwavering patience. By thoroughly understanding the biology of the ACL graft healing timeline, you can make informed, sensible decisions about your daily rehabilitation.
Always remember that your knee is structurally at its absolute weakest between 6 and 12 weeks post-surgery, even if your pain is completely gone and you feel remarkably strong. You must actively protect your graft during this crucial danger window by modifying your physical activities and placing total trust in your rehabilitation team.
Every patient possesses unique anatomy, and every healing process requires a tailored approach. For highly personalised advice and expert orthopaedic care, reach out to Dr Dan Cohen. Seeking professional guidance ensures your recovery remains safely on track, helping you confidently return to the pain-free, active life you deserve.
